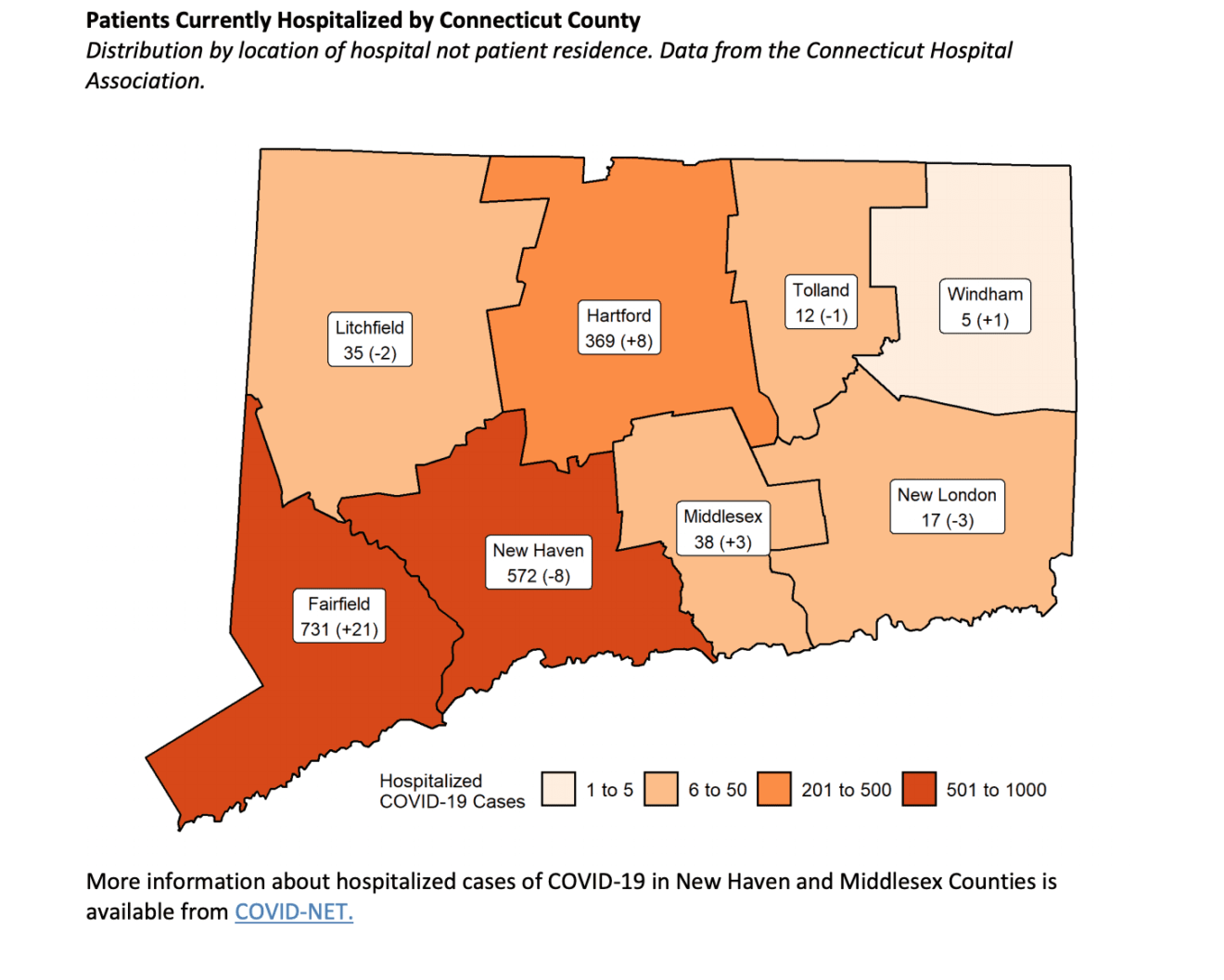
Almost 14,000 people have tested positive for COVID-19 and 671 have died statewide as of Tuesday. Of those deaths, just 28 -- 4 percent -- are in New London and Middlesex county including one in Old ...
Haven’t subscribed yet? Click here to register.
CT Examiner is just $20 a year. And if you want to unsubscribe? That’s online and at the click of a button. No phone calls. No runaround. No hassle.
At less than a tenth the cost of our statewide competitors, our promise to you is no-nonsense federal, state, and local news that’s nonpartisan, respects your privacy and is ad-free.
Subscribe and see why CT Examiner is the fastest growing news source in Connecticut.